Fifteen to twenty years ago, cardiology was the crown jewel of hospital innovation. It was the subspecialty fueling new technologies, driving capital investment, and shaping the image of leading health systems. Today, oncology has eclipsed cardiology as the top revenue generator, commanding a larger share of research dollars, capital budgets, and systemwide focus.
But cardiology is far from fading. In fact, it is poised for a new wave of investment and one shaped not by massive inpatient towers of the past, but by outpatient hubs, multidisciplinary models, digital integration, and preventive care. For architects, the shift opens an important conversation: how do we design spaces that align with where cardiac care is going, not where it has been?
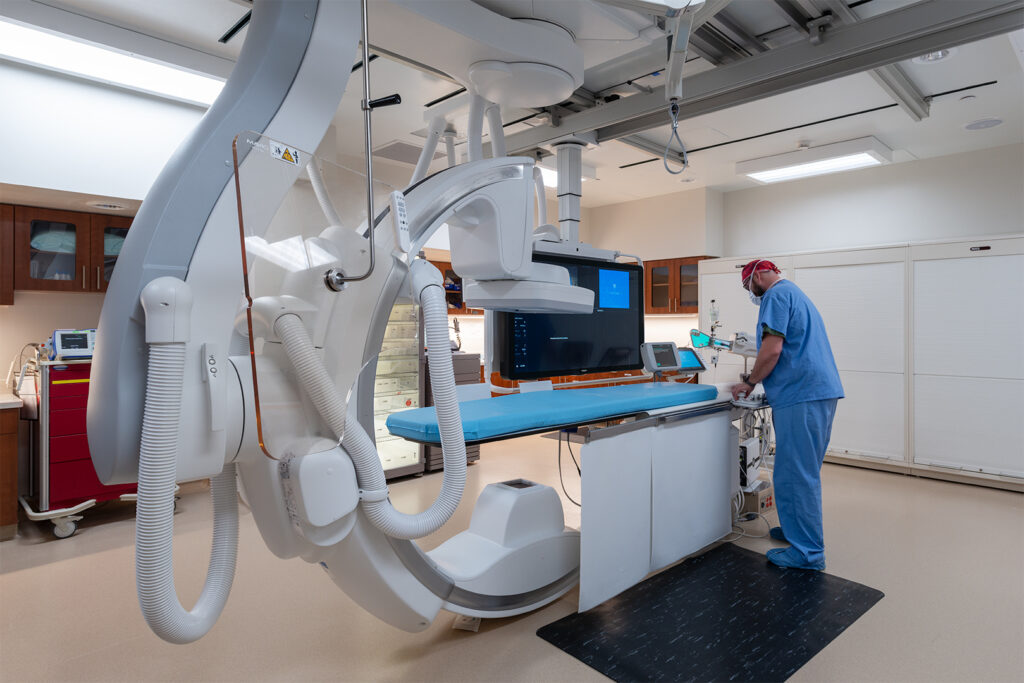
The Outpatient Shift: Cardiac Care Beyond the Hospital Walls
Cardiology is following a well-worn path seen across many service lines: moving procedures into ambulatory surgery centers (ASCs), office-based labs, and outpatient imaging suites. Cath labs, electrophysiology procedures, and non-invasive imaging are increasingly delivered outside the acute-care campus.
Design implication: Outpatient cardiology facilities must balance high-tech environments with smaller, more efficient footprints. Flexible procedure rooms, integrated prep and recovery areas, and patient-friendly circulation can make outpatient centers both cost-effective and highly competitive.
Cardiometabolic Care: The Next Frontier
Obesity, diabetes, and cardiovascular disease are converging in ways that demand integrated care. With GLP-1 medications and SGLT2 inhibitors reshaping treatment protocols, many health systems are rethinking how they deliver cardiometabolic care.
Design implication: Spaces that support multidisciplinary teams, like cardiologists, endocrinologists, nutritionists, and pharmacists, are becoming essential. Education rooms, counseling areas, and pharmacy access points help these centers extend care beyond the clinic visit into long-term prevention.
Imaging as the New Front Door
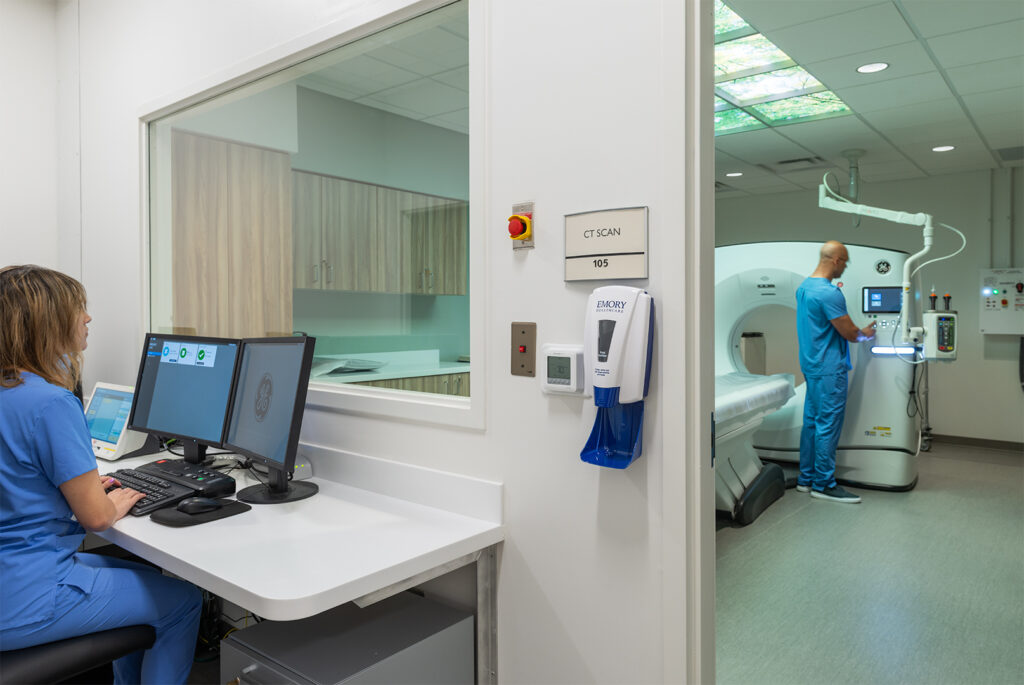
Advanced imaging, such as cardiac CT, MRI, and echocardiography, has become the entry point to many treatment pathways. As imaging volumes rise, throughput and efficiency are paramount.
Design implication: Imaging centers must be designed for speed, comfort, and adaptability. Planning for equipment turnover, optimized prep/recovery flows, and adjacent procedural spaces ensures facilities stay nimble as technology evolves.
The Cardio-Oncology Connection
Cancer remains the dominant investment for health systems, but cardiology is increasingly linked through the subspecialty of cardio-oncology. Cancer therapies can carry significant cardiovascular risks, and protecting patients from those side effects is critical to ensuring continuity of cancer care.
Design implication: Cancer centers and cardiology programs are being strategically co-located. Exam rooms, imaging, and consult areas embedded near infusion suites or radiation areas help streamline care and minimize disruption.
Workforce Realities: Designing for Team-Based Care
A national shortage of cardiologists means hospitals are leaning heavily on advanced practice providers (APPs), nurses, and allied staff. Team-based models, telemedicine consults, and virtual monitoring are no longer fringe. They are the backbone of access.
Design implication: Facilities must create efficient, flexible work environments. Shared workstations, telehealth-enabled exam rooms, and decentralized nurse hubs help stretch limited resources while maintaining a high standard of care.
Structural Heart and EP Programs: Growth with Precision
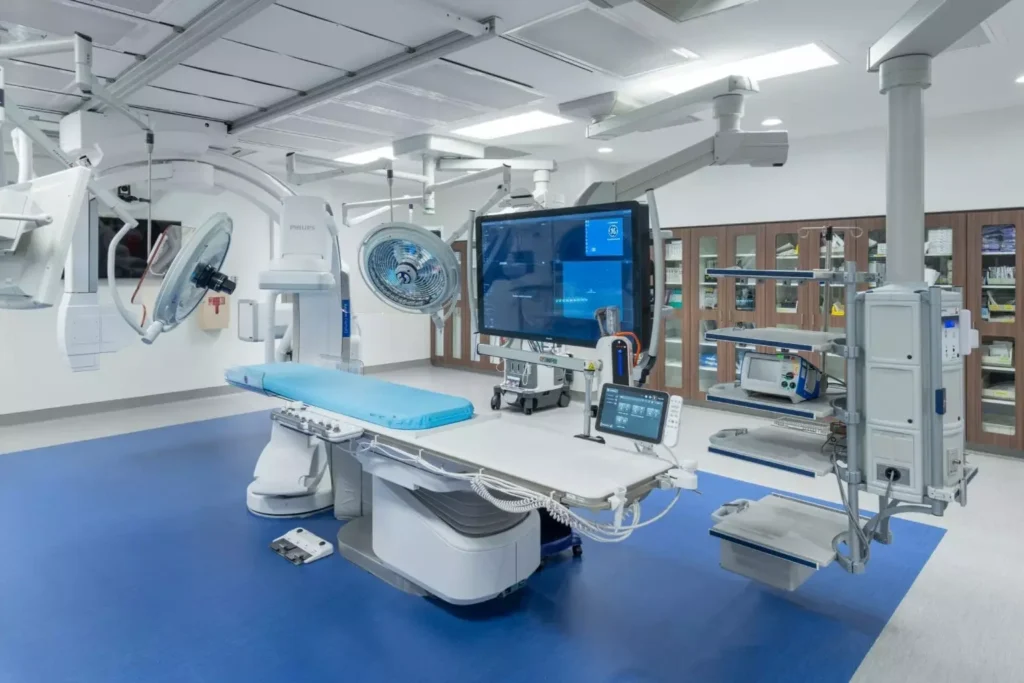
Structural heart and electrophysiology remain high-growth programs, but systems are more selective about where they invest. Instead of blanketing markets with new programs, leaders are targeting facilities where demographics and referral patterns justify the cost.
Design implication: Hybrid ORs, adaptable procedure rooms, and recovery areas that can flex with new devices or techniques ensure investments have longevity.
Digital Infrastructure and AI Integration
Cardiology is among the specialties most impacted by artificial intelligence – from imaging algorithms to predictive analytics. Remote cardiac monitoring is also becoming standard, requiring robust IT infrastructure.
Design implication: Architects must integrate technology readiness into early planning. Data capacity, secure storage, monitoring command centers, and flexible spaces for future digital tools will differentiate hospitals prepared for the next decade.
Prevention as a Design Priority
As new medications and prevention strategies reduce acute events, systems are shifting resources into long-term cardiac wellness. Patient education, nutrition counseling, and lifestyle management programs are becoming critical.
Design implication: Designing for prevention often means smaller, hospitality-inspired spaces such as cafés that double as nutrition classrooms, wellness lounges, or group counseling areas that feel approachable and engaging.
The Architectural Imperative

The future of cardiac care is less about building monumental new hospitals and more about designing environments that are nimble, networked, and strategically aligned with hospital system priorities. For architects, this means:
- Designing for flexibility as technologies and therapies evolve.
- Anticipating adjacencies across service lines, especially between cardiology and oncology.
- Creating outpatient hubs that balance efficiency with a welcoming patient experience.
- Planning for digital infrastructure and remote care from the start.
Conclusion
Cardiology may no longer command the singular spotlight it held two decades ago, but it is entering a new era and one that is defined by outpatient care, cardiometabolic integration, AI-enabled diagnostics, and preventative wellness. For hospital systems, the question is not whether to reinvest in cardiology, but how.
For architects, the opportunity is clear: to design spaces that give health systems the agility to respond to shifting therapies, patient demographics, and workforce realities while keeping cardiac care at the heart of community health for decades to come.




